Morphine is a pain medication of the opiate variety which is found naturally in a number of plants and animals. It acts directly on the central nervous system (CNS) to decrease the feeling of pain. It can be taken for both acute pain and chronic pain. It is frequently used for pain from myocardial infarction and during labour.
Molecular Structure |
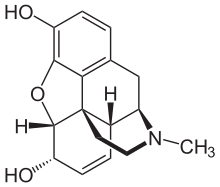
Class of Drug |
Narcotic analgesic, agonist.
Mechanism of Action |
Binds to opiate receptors and blocks ascending pain pathways. Reduces patient’s perception of pain without altering cause of the pain.
Indications / Dosage / Route |
Routes of Administration: Oral, IV and IM.
Condition: Analgesia
Dose: Adults: PO 30-50 mg q4h.
DAdults: Sustained-release tablets 30-100 mg q8-12h.
DAdults: IV, IM 5-20 mg/70 kg q4h.
DChildren: IV, IM 100-200 pg/kg. Maximum: 15 mg
DAdults: IV 2-10 mg/70 kg body wt
Adjustment of Dosage |
Kidney disease: None.
Liver disease: None.
Elderly: Use with caution.
Pediatric: See above.
| Onset of Action | Peak Effect | Duration | |
| IV | 15-60 min | 0.5-1 h | 3-7 h |
Food and Drug Interactions |
Food: May be taken with food to lessen GI upset.
Pregnancy: Category B. Category D if prolonged use or if given in high doses at term.
Lactation: Appears in breast milk. Potentially toxic to infant. Avoid breastfeeding.
Contraindications: Hypersensitivity to narcotics of the same chemical class, respiratory depression in the absence of resuscitation equipment, premature infant, labor prior to delivery of premature infant.
Warnings / Precautions |
> Use with caution in patients with head injury with increased intracranial pressure, serious alcoholism, prostatic hypertrophy, chronic pulmonary disease, severe liver or kidney disease, disorders of biliary tract and postoperative patients with pulmonary disease.
> Administer drug before patient experiences severe pain for fullest efficacy of the drug.
> Have the following available when treating patient with this drug: naloxone (Narcan) or other antagonist, means of administering oxygen, and support of respiration.
> Nausea, vomiting, and orthostatic hypotension occur most prominently in ambulatory patients. If nausea and vomiting persist, it may be necessary to administer an antiemetic, eg, droperidol or prochlorperazine.
> This drug can cause severe hypotension in a patient who is volume depleted or if given along with a phenothiazine or general anesthesia.
> Careful diagnosis must be made of acute abdominal condition before this drug is administered.
Clinically Important Drug Interactions |
> Drugs that increase effects/toxocity of narcotic analgesis: alcohol, benzodiazepines, antihistamines, phenothiazines, butyrophenones, triyclic antidepressants, MAO inhibitors.
Adverse Reactions |
> Common: constipation, lightheadedness, dizziness, sedation, nausea, vomiting, sweating, dysplasia, emphoma.
> Serious: hypotension, bradycardia, apnea, circulatory depression, respiratory arrest, convulsions (high doses, IV), shock, increased intracranial depression, paralytic ileus, physical and psychologic dependence and addiction.
Parameters to Monitor |
> Signs and symptoms of pain: restlessness, anorexia, elevated pulse, increased respiratory rate. Differentiate restlessness associated with pain from that caused by CNS stimulation caused by morphine. This paradoxical reaction is seen mainly in women and elderly patients.
> Respiratory status prior to and following drug administration. Note rate, depth, and rhythm of respirations. If rate falls below 12/min, withhold drug unless patient is receiving ventilatory support. Consider administering an antagonist, eg, naloxone 0.1-0.5 mg IV every 2-3 minutes. Be aware that respiratory depression may occur even at small doses. Restlessness may also be a symptom of hypoxia.
> Character of cough reflex. Encourage postoperative patient to change position frequently (at least every 2 hours), breathe deeply, and cough at regular intervals, unless coughing is contraindicated. These steps will help prevent atelectasis.
> Signs and symptoms of urinary retention, particularly in patients with prostatic hypertrophy or urethral stricture. Monitor output/intake and check for oliguria or urinary retention.
> Signs of tolerance or dependence. Determine whether patient is attempting to obtain more drug than prescribed as this may indicate onset of tolerance and possibility of dependence. If tolerance develops to one opiate, there is generally cross-tolerance to all drags in this class. Physical dependence is generally not a problem if the drag is given <2 weeks.
> BP. If systolic pressure falls below 90 mm Hg, do not administer the drag unless there is ventilatory support. Be aware that the elderly and those receiving drags with hypotensive properties are most susceptible to sharp fall in BP.
> Heart rate. Withhold drag if adult pulse rate is below 60 beats/min. Alternatively, administer atropine.
> Respiratory status of newborn baby and possible withdrawal reaction. If the mother has received an opiate just prior to delivery, the neonate may experience severe respiratory depression. Resuscitation may be necessary as may a narcotic antgonist, eg, Narcan. Alternatively, the neonate may experience severe withdrawal symptoms 1-4 days after birth. In such circumstances, administer tincture of opium or paregoric.
> Signs and symptoms of constipation. If patient is on drag longer than 2-3 days, administer a laxative.
> For patients on long-term therapy, administer a bulk or fiber laxative, eg, psyllium, 1 teaspoon in 240 mL liquid/d. Encourage patient to drink large amounts of fluid, 2.5 to 3 L/d.
Advice to Patient |
> Avoid alcohol and other CNS depressants such as sedatives (eg, diazepam) when taking this drug.
> Avoid driving and other activities requiring mental alertness or that are potentially dangerous until response to drug is known.
> Change position slowly, in particular from recumbent to up-right, to minimize orthostatic hypotension. Sit at the edge of the bed for several minutes before standing, and he down if feeling faint or dizzy. Avoid hot showers or baths and standing for long period. Male patients should sit on the toilet while urinating rather than standing.
> Do not increase dose if you are not experiencing sufficient pain relief without approval from treating physician.
> Do not stop medication abruptly when you have been taking it for >2 weeks. If so, a withdrawal reaction may occur within 24-48 hours. The following are typical symptoms: irritability, perspiration, rhinorrhea, lacrimation, dilated pupil, piloerection (“goose flesh”), bone and muscle aches, restless sleep (“yen”), increased systolic pressure, hyperpyrexia, diarrhea, hyperglycemia, spontaneous orgasm.
> Do not take OTC drugs without approval by treating physician. Some of these may potentiate the CNS depressant effects of the drug.
> If dizziness persists more than 3 days, decrease dose gradually (over 1-2 days).
> Attempt to void every 4 hours.
Further Useful Info |
> Morphine is the drag of choice for the following conditions: treatment of severe pain, pain of terminal cancer when treatment with other drags is not effective, noncancer pain when treatment with other drugs is not effective, postoperative pain, postmyocardial pain, pulmonary edema.
> The following considerations should be made in the event of pain or in unusual circumstances, eg, breakthrough pain: use a sustained release morphine preparation along with one that provides rapid release. Transdermal therapy may be beneficial.
> Cancer patients who are experiencing severe, unrelieved pain: Administer the drag IV or IM and switch to oral therapy once pain is controlled. Transdermal therapy may be beneficial.


