Atenolol is a selective β1 receptor antagonist, a drug belonging to the group of beta blockers (sometimes written β-blockers), a class of drugs used primarily in cardiovascular diseases. Introduced in 1976, atenolol was developed as a replacement for propranolol in the treatment of hypertension. It works by slowing down the heart and reducing its workload.
Molecular Structure |
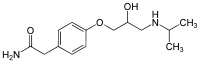
Class of Drug |
β-Adrenergic receptor blocker.
Mechanism of Action |
Competitive blocker of β-adrenergic receptors in heart and blood vessels.
Indications / Dosage / Route |
Routes of Administration: Oral and IV.
Condition: Hypertension
Dose: Adults Initial: PO 50 mg/d. Maximum: 100 mg/d.
Condition: Angina
Dose: Initial: PO 50 mg/d. Maintenance: 100-200 mg/d
Condition: Ventricular arrhythmias
Dose: Adults PO 50-100 mg/d.
Condition: Acute MI
Dose: Adults IV 5 mg over 5 min, followed by second 5-mg dose 10 min later; then 50-mg tablet 10 min after last IV dose, then another 50-mg dose 12 hours later, then 100 mg/d or 50 mg b.i.d. for 6-9 days.
Adjustment of Dosage |
Kidney disease: creatinine clearance 15-35 mL/min: 50 mg/d; creatinine clearance <15 mL/min : 25 mg/d.
Liver disease: None.
Elderly: None
Pediatric: Safety and efficacy have not been established in children.
Food and Drug Interactions |
Food: No restriction
Pregnancy: Category B.
Lactation: Appears in breast milk. Considered compatible by the American Academy of Pediatrics. Observe infant for hypotension, bradycardia, cyanosis.
Contraindications: Cardiogenic shock, asthma, CHF unless it is secondary to tachyarrhythmia treated with a β blocker, sinus bradycardia and AV block greater than first degree, severe COPD.
Warnings / Precautions |
> Use with caution in patients with the following conditions: diabetes, kidney disease, liver disease, COPD, peripheral vascular disease.
> Do not stop drug abruptly as this may precipitate arrhythmias, angina, MI or cause rebound hypertension. If necessary to discontinue, taper as follows: Reduce dose by 25-50% and reassess after 1-2 weeks. If status is unchanged, reduce by another 50% and reassess after 1-2 weeks.
> Drug may mask the symptoms of hyperthyroidism, mainly tachycardia.
> Drug may exacerbate symptoms of arterial insufficiency in patients with peripheral or mesenteric vascular disease.
Clinically Important Drug Interactions |
> Drugs that increase effects/toxicity of β blockers: reserpine, bretylium, calcium channel blockers.
> Drugs that decrease effects/toxicity of β blockers: aluminum salts, calcium salts, cholestyramine, barbiturates, NSAIDs, rifampin.
Adverse Reactions |
> Common: fatigue, headache, impotence.
> Serious: symptomatic bradycardia, CHF, pulmonary edema.
Parameters to Monitor |
> Liver enzymes, serum BUN and creatinine, CBC with differential and platelets.
> Pulse rate near end of dosing interval or before the next dose is taken. A reasonable target is 60-80 bpm for resting apical ventricular rate. If severe bradycardia develops, consider treatment with glucagon, isoproterenol, IV atropine (1-3 mg in divided doses). If hypotension occurs despite correction of bradycardia, administer vasopressor (norephinephrine, dopamine, or dobutamine).
> Symptoms of CHF. Digitalize patient and administer a diuretic or glucagon.
> Efficacy of treatment: decreased BP, decreased number and severity of anginal attacks, improvement in exercise tolerance. Confirm control of arrhythmias by ECG, apical pulse, BP, circulation in extremities, and respiration. Monitor closely when changing dose.
> CNS effects. If patient experiences mental depression reduce dosage by 50%. The elderly are particularly sensitive to adverse CNS effects.
> Signs of bronchospasm. Stop therapy and administer large doses of (t-adreneigic bronchodilator, eg, albuterol, terbutaline, or aminophylline.
> Signs of cold extremities. If severe, stop drug. Consider β blocker with sympathomimetic property
Advice to Patient |
> Avoid driving and other activities requiring mental alertness or that are potentially dangerous until response to drug is known.
> Change position slowly, in particular from recumbent to upright, to minimize orthostatic hypotension. Sit at the edge of the bed for several minutes before standing, and lie down if feeling faint or dizzy. Avoid hot showers or baths and standing for long periods. Male patients should sit on the toilet while urinating rather than standing.
> Dress warmly in winter and avoid prolonged exposure to cold as drug may cause increased sensitivity to cold.
> Avoid drinks that contain xanthines (caffeine, theophylline, theobromine) including colas, tea, and cocoa because they may counteract effect of drug.
> Restrict dietary sodium to avoid volume expansion.
> Drug may blunt response to usual rise in BP and chest pain under stressful conditions such as vigorous exercise and fever.
Further Useful Info |
> Stopping a β blocker before surgery is controversial. Some advocate discontinuing the drug 48 hours before surgery; others recommend withdrawal for a considerably longer time. Notify anesthesiologist that patient has been on β blocker.
> β blockers are drugs of first choice for hypertension, particularly in patients with the following conditions: previous MI, ischemic heart disease, aneurysm, atrioventricular arrhythmias, migraine. These drugs are also first choice for chronic stable angina, used in conjunction with nitroglycerin.
> Following a MI, patients should be administered a β blocker.
> β blockers are considered to be first-line drugs for prophylaxis of migraine headache in patients who have two or more attacks per month.


