Streptomycin is an antibiotic used to treat a number of bacterial infections. This includes tuberculosis, Mycobacterium avium complex, endocarditis, brucellosis, Burkholderia infection, plague, tularemia, and rat bite fever. For active tuberculosis it is often given together with isoniazid, rifampicin, and pyrazinamide.
Molecular Structure |
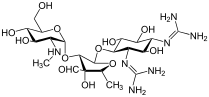
Class of Drug |
Antibiotic, aminoglycoside.
Mechanism of Action |
Binds to ribosomal units in bacteria, inhibits protein synthesis.
Susceptible organisms in vivo: Mycobacterium tuberculosis, Yersinia pestis, Francisella tularensis, Brucella synergism against enterococci and streptococcoi.
Indications / Dosage / Route |
Routes of Administration: IM only.
Condition: Inguinal granuloma, chancroid; respiratory, endocardial, meningeal infections (Hemophilus influenzae), pneumonia, UTIs, bacteremia (gram negative bacillary)
Dose: Adults: 15 mg/kg/d. Maximum: 1 g/d.
Children: 20-40 mg/kg/d. Maximum: 1 g/d.
Condition: Tuberculosis
Dose: Adults: 1 g or 15 mg/kg/d, 2-3 months, then 1 g 2-3 times/wk. Maximum: 1 g/d.
Children: IM 20-40 mg/kg/d. Maximum: 1 g/d.
Condition: Tularemia
Dose: Adults: 1-2 g/d in divided doses, 7-14 days
Condition: Plague
Dose: Adults: 2 g/d in 2 divided doses, minimum 10 days.
Condition: Streptococal endocarditis (for synergism with a β-lactam)
Dose: Adults Initial: 1 g b.i.d. (first week), then 500 mg b.i.d. second week.
Condition: Enterococcal endocarditis (with penicillin) (for synergism with ampicillin or vancomycin)
Dose: Initial: 1 g b.i.d. (2 weeks), then 5 mg b.i.d. next 4 weeks.
Adjustment of Dosage |
Kidney disease: Creatinine clearance 10-50 mL/min: administration interval 24-72 hours; creatinine clearance <10 mL/ min: administration interval 72-96 hours.
Liver disease: None.
Elderly: None
Pediatric: See above.
Food and Drug Interactions |
Food: No restrictions.
Pregnancy: Category D.
Lactation: Appears in breast milk. Considered compatible by American Academy of Pediatrics.
Contraindications: Elypersensitivity to aminoglycoside antibiotics.
Warnings / Precautions |
> Use with caution in patients with renal disease, neuromuscular disorders (eg, myasthenia gravis, parkinsonism), hearing disorders.
> Do not combine this drug with any other drug in the same IV bag.
Clinically Important Drug Interactions |
> Drugs that increase effects/toxicity of aminoglycosides: loop diuretics, amphotericin B, enflurane, vancomycin, NSAIDs.
> Drugs that decrease effects/toxicity of aminoglycosides: penicillins (high dose), cephalosporins.
Adverse Reactions |
> Common: None.
> Serious: renal toxicity, ototoxicity, neuromuscular paralysis, respiratory depression (infants), superinfection
Parameters to Monitor |
> Peak and trough serum levels 48 hours after beginning therapy and every 3-4 days thereafter as well as after changing doses. Peak (therapeutic): = 15—40 μg/mL; trough: <4 μg/mL.
> Signs of ototoxicity: tinnitus, vertigo, hearing loss. The drug should be stopped if tinnitus or vertigo occurs. Limit administration to 7-10 days to decrease the risk of ototoxicity.
> Renal function periodically. If serum creatinine increases by more than 50% over baseline value, it may be advisable to discontinue drug treatment and use a less nephrotoxic agent, eg, a quinolone or cephalosporin.
> Efficacy of drug action. If there is no response in 3-7 days, reculture and consider another drug.
> Neuromuscular function when administering the drug IV. Too rapid administration may cause paralysis and apnea. Have calcium gluconate or pyridostigmine available to reverse such an effect.
> Neurologic status if the drug is given for hepatic encephalopathy.
> Signs and symptoms of allergic reaction.
Further Useful Info |
> Streptomycin has the greatest activity of all the aminoglycosides against M. tuberculosis. It is a first-line drug for tuberculosis though not as effective as isoniazid and rifampin.
> Streptomycin is the drug of choice to treat plague and brucellosis.
> Streptomycin and gentamicin are the drugs of choice to treat tularemia.



