Norfloxacin is a synthetic antibacterial agent that belongs to the class of fluoroquinolone antibiotics. It is used to treat urinary tract infections, gynecological infections, inflammation of the prostate gland, gonorrhea and bladder infection. Eye drops were approved for use in children older than one year of age.
Molecular Structure |
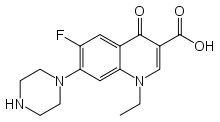
Class of Drug |
Broad-spectrum quinolone antibiotic.
Mechanism of Action |
Inhibits DNA gyrase, thereby blocking bacterial DNA replication.
Susceptible organisms in vivo: Citrobacter sp, Enterobacter sp, Escherichia coli, Klebsiella pneumoniae, Neisseria gonorrhoeae, Proteus mirabilis, Proteus vulgaris, Pseudomonas aeruginosa (variable), Serratia marcescens, Staphylococcus aureus (less than ciprofloxacin), Staph, epidermidis, Staph, hemolyticus, Staph. saprophyticus, staph, agalactiae, Streptococcus faecalis.
Indications / Dosage / Route |
Routes of Administration: Oral only.
Condition: Uncomplicated UTIs (E. coli, K. pneumoniae, P. mirabilis)
Dose: Adults: 400 mg ql2h, 3 days.
Condition: Uncomplicated UTIs caused by other indicated organisms
Dose: Adults: 400 mg ql2h, 7-10 days.
Condition: Uncomplicated UTIs
Dose: Adults: 400 mg ql2h, 10-21 days.
Condition: Uncomplicated gonorrhea
Dose: Adults: 800 mg, single dose
Condition: Prostatis, acute or chronic
Dose: Adults 400 mg ql2h, 28 days.
Adjustment of Dosage |
Kidney disease: Creatinine clearance <30 mL/min: 400 mg q day, 4-7 days.
Liver disease: None.
Elderly: None
Pediatric: Safety and efficacy have not been established in children <18 years.
Food and Drug Interactions |
Food: Take 1 hour before or 2 hours after meals with a glass of water.
Pregnancy: Category C.
Lactation: Likely to appear in breast milk. Potentially toxic to infant. Avoid breastfeeding.
Contraindications: Hypersensitivity to fluoroquinolone or quinolone antibiotics.
Warnings / Precautions |
> Use with caution in patients with CNS disorders (epilepsy), kidney disease.
> Therapy should be continued for 2-4 days after symptoms have disappeared.
> Achilles and other tendon rupture have occurred in patients taking fluoroquinolones.
> Serious and fatal hypersensitivity reactions have occurred with these drugs, even after the first dose.
> Reserve use of this drug for infections that are difficult to treat by other means.
Clinically Important Drug Interactions |
> Drugs that increase effects/toxicity of fluoroquinolones: cyclosporine, probenecid.
> Dmgs that decrease effects/toxicity of fluoroquinolones: antacids, antineoplastic agents, didanosine, sucralfate, iron salts, zinc salts, caffeine.
> Fluoroquinolones increase effects/toxicity of oral anticoagulants, theophylline, caffeine
Adverse Reactions |
> Common: None.
> Serious: Hypersensitivity reaction (anaphylaxis), seizures, pseudomembranous colitis, cholestatic jaundice, renal failure, pulmonary edema, pulmonary embolism, cardiovascular collapse, pharyngeal edema
Parameters to Monitor |
> Renal, hepatic, and hemopoietic systems should be monitored periodically during prolonged therapy.
> Intake of fluids and urinary and other fluid output to minimize renal toxicity. Increase fluid intake if inadequate. Closely monitor electrolyte levels.
> Signs of hypersensitivity reactions.
> Signs and symptoms of antibiotic induced bacterial or fungal superinfection: Use of yogurt (4 oz/d) may be helpful in prevention of superinfection.
> Signs and symptoms of tendon pain. These may be an indication of tendon rupture.
> Monitor patients for evidence of development of microbial resistance with loss of effectiveness.
Advice to Patient |
> Limit intake of caffeinated products including coffee and colas.
> Drink a great deal of fluids during therapy with this drug.
> Do not undertake strenuous exercise while taking this drug.
> To minimize possible photosensitivity reaction, apply adequate sunscreen and use proper covering when exposed to strong sunlight.
Further Useful Info |
> Use of norfloxacin is limited to treatment of UTI, prostatitis, and uncomplicated gonorrhea.
> This drug is recommended as an alternative to aminoglyco sides when clinically relevant.


