Enalapril is a medication used to treat high blood pressure, diabetic kidney disease, and heart failure. For heart failure it is generally used with a diuretic such as furosemide. It is given by mouth or injection into a vein.
Molecular Structure |
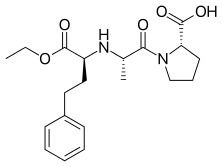
Class of Drug |
ACE inhibitor.
Mechanism of Action |
Inhibits ACE, thereby preventing conversion of angiotensin I to angiotensin II, resulting in decreased peripheral arterial resistance.
Indications / Dosage / Route |
Routes of Administration: Oral and IV.
Condition: Hypertension
Dose: Adults: Initial PO 5 mg/d.
Condition: CHF
Dose: Adults: Initial PO 2.5 mg/d or b.i.d. Maintenance: 5 mg/d.
Adults: IV 0.625-1.25 mg q6h.
Adjustment of Dosage |
Kidney disease: Creatinine clearance >30mL/min: none; creatinine clearance <30mL/min: Initial 2.5 mg/d, maximum 40 mg/d.
Liver disease: None.
Elderly: None
Pediatric: Safety and efficacy have not been established.
| Onset of Action | Peak Effect | Duration |
| PO:1 h IV:15 min | 4-6 h 1-4 h | 24 h 6 h |
Food and Drug Interactions |
Food: Administer without regard to meals.
Pregnancy: Category C for first trimester. Category D for second and third trimesters.
Lactation: Appears in breast milk. Considered compatible by American Academy of Pediatrics.
Contraindications: Hypersensitivity to ACE inhibitors, hereditary or ideopathic angioedema, second and third trimesters of pregnancy.
Warnings / Precautions |
> Use with caution in patients with the following conditions: kidney disease especially renal artery stenosis, drugs that cause bone marrow depression, hypovolemia, hyponatremia, cardiac or cerebral insufficiency, collagen vascular disease, lupus erythematosus, scleroderma, patients undergoing dialysis.
> ACE inhibitors have been associated with anaphylaxis and angioedema.
> Use extreme caution in combination with potassium-sparing diuretics (high risk of hyperkalemia).
> Sodium or volume-depleted patients may experience severe hypotension. Lower initial doses are advised.
> During surgery/anesthesia, the drug may increase hypotension. Volume expansion may be required.
> There may be a profound drop in BP after the first dose is taken. Close medical supervision is necessary once therapy is begun.
Clinically Important Drug Interactions |
> Enalapril increases toxicity of the following drugs: lithium, azothioprine, allopurinol, potassium-sparing diuretics, digoxin.
> Drugs that increase toxicity of enalapril: potassium-sparing drugs, phenothiazines (eg, chlorpromazine).
> Drugs that decrease effectiveness of enalapril: NSAIDs, ant-acids, cyclosporine.
Adverse Reactions |
> Common: None.
> Serious: Bone marrow depression (neutropenia, agranulocytosis), hypotension, angioedema, hyperkalemia, oliguria, chest pain, angina, tachycardia, asthma, bronchospasm, autoimmune symptom complex (see Editorial Comments), hepatitis, liver failure.
Parameters to Monitor |
> Electrolytes, CBC with differential and platelets, BUN and creatinine.
> Signs and symptoms of angioedema: swelling of face, lips, tongue, extremities, glottis, larynx. Observe in particular for obstruction of airway, difficulty in breathing. If symptoms are not relieved by an antihistamine, discontinue drug.
> Patient’s BP closely, particularly at beginning of therapy. Observe for evidence of severe hypotension. Patients who are hypovolemic as a result of GI fluid loss or diuretics may exhibit severe hypotension. Also monitor for orthostatic changes.
> Signs of persistent, nonproductive cough; this may be drug induced.
> Changes in weight in patients with CHF. Gain of more than 2 kg/wk may indicate development of edema.
> Signs and symptoms of infection.
> Possible antinuclear antibody development.
> Monitor WBC count monthly (first 3-6 months) and at frequent intervals thereafter for patients with collagen vascular disease or renal insufficiency. Discontinue therapy if neutrophil count drops below 1000.
> Signs and symptoms of bone marrow depression.
> Intake of fluids and urinary and other fluid output to minimize renal toxicity. Increase fluid intake if inadequate. Closely monitor electrolyte levels.
> Signs and symptoms of renal toxicity.
Advice to Patient |
> Do not use salt substitutes containing potassium.
> Use two forms of birth control including hormonal and barrier methods.
> Avoid NSAIDs; may be present in OTC preparations.
> Take BP periodically and report to treating physician if significant changes occur.
> Stop drug if the following occurs: prolonged vomiting or diarrhea. These symptoms may indicate plasma volume reduction.
> Discontinue drug immediately if signs of angioedema (swelling of face, lips, extremities, breathing or swallowing difficulty) become prominent, and notify physician immediately if this occurs.
> If chronic cough develops, notify treating physician.
Further Useful Info |
> Unlabeled uses of ACE inhibitors include hypertensive crisis, diagnosis of renal artery stenosis, hyperaldosteronism, Raynaud’s phenomenon, angina, diabetic nephropathy.
> ACE inhibitors have been associated with an autoimmune type symptom complex including fever, positive antinuclear antibody, myositis, vasculitis, and arthritis.
> Typically twice-a-day administration is favorable but it may be used once daily even at higher doses.
> The ACE inhibitors have been highly efficacious and well tolerated class of drug. Nearly every large randomized clinical trial examining their use has been favorable. First, the Consensus Trial proved that enalapril decreased mortality and increased quality of life in Class II and HI CHF patients. Then the Solve trial and others proved their benefits in remodeling myocardium post MI. The DCCT trial of diabetic patients demonstrated the ability of ACE inhibitors to decrease the small vessel damage to retinas and glomeruli. Clinical trials looking into primary prevention of cardiac effects are ongoing. Treatment with this class of drug is the gold standard in patients with left ventricular systolic dysfunction. The two most common adverse effects of ACE inhibitors are cough and angioedema. Transient and persistent rises in antinuclear antibodies have been noted. As this class of drug is a vasodilator, orthostasis is another potential problem.


