This discussion covers the following information related to Congestive Heart Failure (CHF):
- Congestive Heart Failure (CHF) or Heart Failure (HF)
- Signs and Symptoms of Congestive Heart Failure
- Causes of Congestive Heart Failure
- Risk Factors for CHF
- Complications of Heart Failure
- Tests and Diagnosis for Congestive Heart Failure
- Treatment and Drugs for CHF
Congestive Heart Failure Definition
Heart failure, sometimes known as congestive heart failure, occurs when your heart muscle doesn’t pump blood as well as it should. Certain conditions, such as narrowed arteries in your heart (coronary artery disease) or high blood pressure, gradually leave your heart too weak or stiff to fill and pump efficiently.
Not all conditions that lead to heart failure can be reversed, but treatments can improve the signs and symptoms of heart failure and help you live longer. Lifestyle changes — such as exercising, reducing salt in your diet, managing stress and losing weight — can improve your quality of life.
One way to prevent heart failure is to control conditions that cause heart failure, such as coronary artery disease, high blood pressure, diabetes or obesity.
Signs and Symptoms of Congestive Heart Failure
Heart failure can be ongoing (chronic), or your condition may start suddenly (acute).
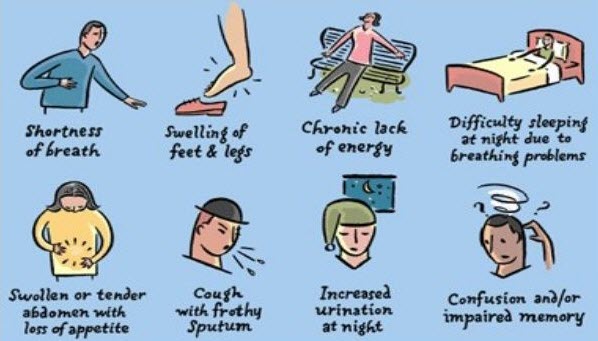
Heart failure signs and symptoms may include:
- Shortness of breath (dyspnea) when you exert yourself or when you lie down
- Fatigue and weakness
- Swelling (edema) in your legs, ankles and feet
- Rapid or irregular heartbeat
- Reduced ability to exercise
- Persistent cough or wheezing with white or pink blood-tinged phlegm
- Increased need to urinate at night
- Swelling of your abdomen (ascites)
- Sudden weight gain from fluid retention
- Lack of appetite and nausea
- Difficulty concentrating or decreased alertness
- Sudden, severe shortness of breath and coughing up pink, foamy mucus
- Chest pain if your heart failure is caused by a heart attack
EMERGENCY CASE See your doctor if you think you might be experiencing signs or symptoms of heart failure. Seek emergency treatment if you experience any of the following: Although these signs and symptoms may be due to heart failure, there are many other possible causes, including other life-threatening heart and lung conditions. Don’t try to diagnose yourself. Call 911 or your local emergency number for immediate help. Emergency room health care providers will try to stabilize your condition and determine if your symptoms are due to heart failure or something else. If you have a diagnosis of heart failure and if any of the symptoms suddenly become worse or you develop a new sign or symptom, it may mean that existing heart failure is getting worse or not responding to treatment. Contact your doctor promptly.
Causes of Congestive Heart Failure

Heart failure often develops after other conditions have damaged or weakened your heart. However, the heart doesn’t need to be weakened to cause heart failure. It can also occur if the heart becomes too stiff.
In heart failure, the main pumping chambers of your heart (the ventricles) may become stiff and not fill properly between beats. In some cases of heart failure, your heart muscle may become damaged and weakened, and the ventricles stretch (dilate) to the point that the heart can’t pump blood efficiently throughout your body. Over time, the heart can no longer keep up with the normal demands placed on it to pump blood to the rest of your body.
An ejection fraction is an important measurement of how well your heart is pumping and is used to help classify heart failure and guide treatment. In a healthy heart, the ejection fraction is 50 percent or higher — meaning that more than half of the blood that fills the ventricle is pumped out with each beat. But heart failure can occur even with a normal ejection fraction. This happens if the heart muscle becomes stiff from conditions such as high blood pressure.
The term “congestive heart failure” comes from blood backing up into — or congesting — the liver, abdomen, lower extremities and lungs. However, not all heart failure is congestive. You might have shortness of breath or weakness due to heart failure and not have any fluid building up.
Heart failure can involve the left side (left ventricle), right side (right ventricle) or both sides of your heart. Generally, heart failure begins with the left side, specifically the left ventricle — your heart’s main pumping chamber.
| Type of Heart Failure | Description |
| Left-sided heart failure | Fluid may back up in your lungs, causing shortness of breath |
| Right-sided heart failure | Fluid may back up into your abdomen, legs and feet, causing swelling |
| Systolic heart failure | The left ventricle can’t contract vigorously, indicating a pumping problem |
| Diastolic heart failure (also called heart failure with preserved ejection fraction) | The left ventricle can’t relax or fill fully, indicating a filling problem |
Any of the following conditions can damage or weaken your heart and can cause heart failure. Some of these can be present without your knowing it:
Coronary artery disease and heart attack: Coronary artery disease is the most common form of heart disease and the most common cause of heart failure. Over time, arteries that supply blood to your heart muscle narrow from a buildup of fatty deposits — a process called atherosclerosis. The buildup of plaques can cause reduced blood flow to your heart.
A heart attack occurs if plaques formed by the fatty deposits in your arteries rupture. This causes a blood clot to form, which may block blood flow to an area of the heart muscle, weakening the heart’s pumping ability and often leaving permanent damage. If the damage is significant, it can lead to a weakened heart muscle.
High blood pressure (hypertension): Blood pressure is the force of blood pumped by your heart through your arteries. If your blood pressure is high, your heart has to work harder than it should to circulate blood throughout your body.
Over time, the heart muscle may become thicker to compensate for the extra work it must perform. Eventually, your heart muscle may become either too stiff or too weak to effectively pump blood.
Faulty heart valves: The valves of your heart keep blood flowing in the proper direction through the heart. A damaged valve — due to a heart defect, coronary artery disease or heart infection — forces your heart to work harder to keep blood flowing as it should.
Over time, this extra work can weaken your heart. Faulty heart valves, however, can be fixed or replaced if found in time.
Damage to the heart muscle (Cardiomyopathy): Heart muscle damage (cardiomyopathy) can have many causes, including several diseases, infections, alcohol abuse and the toxic effect of drugs, such as cocaine or some drugs used for chemotherapy.
Genetic factors play an important role in several types of cardiomyopathy, such as dilated cardiomyopathy, hypertrophic cardiomyopathy, arrhythmogenic right ventricular cardiomyopathy, left ventricular noncompaction and restrictive cardiomyopathy.
Myocarditis: Myocarditis is an inflammation of the heart muscle. It’s most commonly caused by a virus and can lead to left-sided heart failure.
Heart defects you’re born with (congenital heart defects): If your heart and its chambers or valves haven’t formed correctly, the healthy parts of your heart have to work harder to pump blood through your heart, which, in turn, may lead to heart failure.
Abnormal heart rhythms (heart arrhythmias): Abnormal heart rhythms may cause your heart to beat too fast, which creates extra work for your heart. Over time, your heart may weaken, leading to heart failure. A slow heartbeat may prevent your heart from getting enough blood out to the body and may also lead to heart failure.
Other diseases: Chronic diseases — such as diabetes, HIV, hyperthyroidism, hypothyroidism, or a buildup of iron (hemochromatosis) or protein (amyloidosis) —also may contribute to heart failure.
Causes of acute heart failure include viruses that attack the heart muscle, severe infections, allergic reactions, blood clots in the lungs, the use of certain medications or any illness that affects the whole body.


